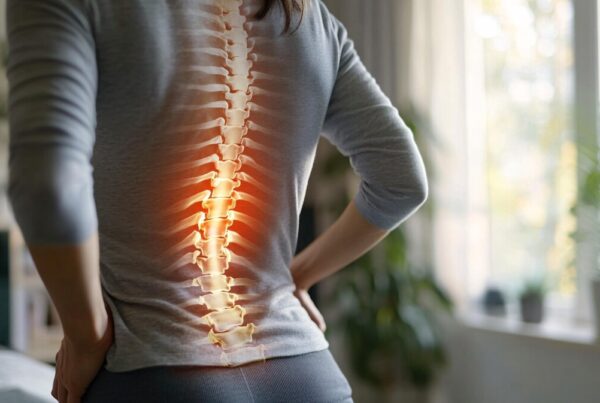
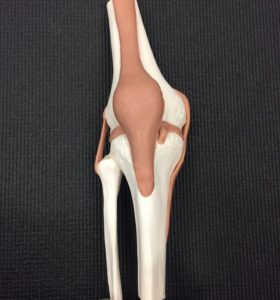
 Recurrent patella subluxations occur when the patella (knee cap) is forced out of its natural setting in the trochlear groove of the femur (thigh) bone, and then relocates back into the groove again. Patella subluxation can be traumatic, caused by a force against the knee such as a contact sport injury, or atraumatic, occurring with much less force involved . I’ve had a few patients recently who’ve suffered this injury, both on and off the rugby field, so it can affect people of all activity levels. One of my patient’s was merely sitting cross-legged during her exercises class and her kneecap “popped” out and back into place.
Recurrent patella subluxations occur when the patella (knee cap) is forced out of its natural setting in the trochlear groove of the femur (thigh) bone, and then relocates back into the groove again. Patella subluxation can be traumatic, caused by a force against the knee such as a contact sport injury, or atraumatic, occurring with much less force involved . I’ve had a few patients recently who’ve suffered this injury, both on and off the rugby field, so it can affect people of all activity levels. One of my patient’s was merely sitting cross-legged during her exercises class and her kneecap “popped” out and back into place.
So what are some of the factors that lead to a patella subluxation? These include:
– muscle weakness around the knee
– ligament laxity and a loose medial patella retinaculum
– a shallow femoral groove for the kneecap to sit in
– a high sitting patella (patella alta)
– valgus knees (knock knees)
– poor lower limb biomechanics putting more strain on the knee
– poor balance, pelvic & core stability
– gender – females more likely than males
– fatigue
– trauma – a large force knocking the patella out of it’s position
When the patella is moved out of it’s natural trochlear groove of the femur, damage to the soft tissues that hold the patella in it’s position commonly occurs. More frequently, the patella will sublux laterally (outwards) than medially (inwards). Symptoms of a subluxation can include varying degrees of swelling, pain and a feeling as if the knee cap might “pop”” back out again.
The frustrating feature about a subluxing patella is, once its happened, it’s unfortunately more than likely to re-occur as a result of the weakened and loosened structures surrounding the knee cap. There is between a 15-45% chance of subluxing your patella again straight after the initial incidence, and a 60-80% chance of recurrence if you’ve subluxed your patella twice. The patella will normally go back into place depending on the degree of damage caused. In the case of a dislocated patella when the kneecap does not immediately return to its proper position, the knee may need to be moved into extension/straightened to help relocate the patella.
As you can imagine, reducing the risk of recurrence requires a thorough process of assessment, treatment and rehabilitation. Surgery will sometimes be required if there is extensive soft tissue damage or any fractured pieces of bone, or if an individual suffers multiple subluxations as a result of an inherited trait such as a shallow femoral groove or a high sitting patella. This is usually required when conservative treatment is no longer achieving results. Surgery is generally never used as the first intervention as the complications of surgery can include infection, thrombosis, delayed bone healing and ongoing knee pain. Alternatively, after the initial management of pain and swelling, Physiotherapy is required to address risk factors and prevent recurrence.
Physiotherapy will be used to help:
– immobilise the knee cap if required in the initial stages
– lengthen tightened structures that are adding extra pull on the patella, in most cases this includes the iliotibial band, lateral retinaculum and lateral quadriceps muscle
– strengthen weak structures that are required to hold the patella in a better position such as the vastus medialis muscle (VMO) and adductor muscle group
– address pre-disposing factors leading to the original subluxation
– assess the need for orthotics to help improve lower limb biomechanics, amongst other strengthening exercises
– taping of the knee cap may also be used to help return the individual back to the sport of their choice or even for comfort
If you have an “unhappy knee” be sure to book an appointment at one of our Sydney CBD Bend + Mend clinics, to ensure a thorough sports physiotherapy assessment and rehabilitation program is provided.