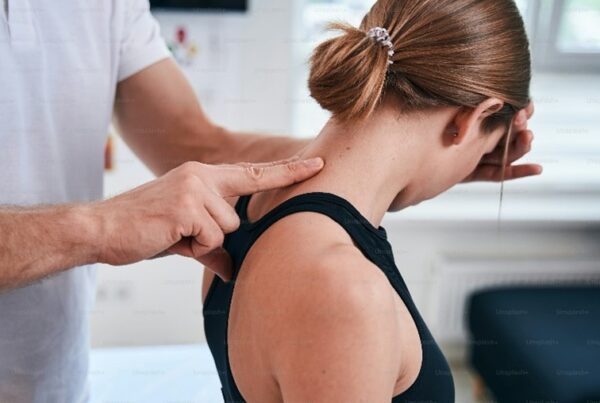
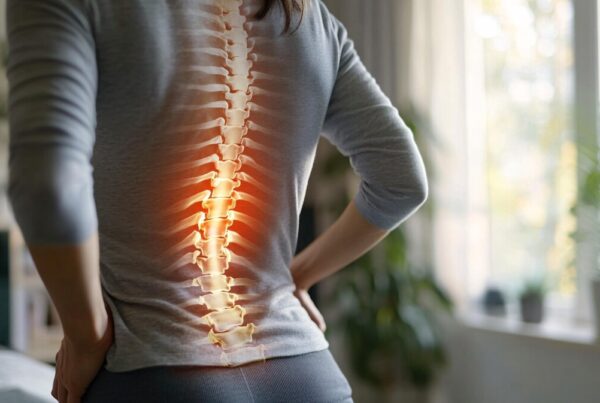
We’ve heard it before – people might assume that if a scan shows any sign of arthritis that their joints are down to ‘bone on bone’, but what does that really mean?
The cartilage in our joints, although designed to absorb shock and load, unfortunately doesn’t heal well. In arthritis, the cartilage first becomes dehydrated and eventually more brittle and unable to cope as well with a normal load such as walking. Small pieces can begin to crack and chip away over time and eventually the cartilage becomes thin and some of the joint surface may have no cartilage left to absorb load. As bone wasn’t designed to absorb shock, it swells, resulting in joint pain. The muscles around the joint are also affected because of changes to the way you move in response to reduced shock absorption and pain.
So, is it really “bone on bone?” For most people, the answer is no.
Arthritis progresses slowly and in many people never gets to the point where their cartilage is completely worn out. Although cartilage loss is a prominent feature of arthritis, contemporary models recognise that the entire joint organ is affected, including meniscal degeneration, a synovial inflammatory response, and bone and cartilage overgrowth (osteophytes). From a biological perspective much of the pain you experience is due to swelling and involves all the structures of the joint. So, even when your scans show arthritis, you still have cartilage left in your joint!
So, what does that mean for you?
Well, the best research we have on early stages of arthritis suggests that exercise is the best treatment. You may be surprised because walking and exercise can make you feel worse, but the key is to find a type of exercise that suits you and doesn’t overload your joints.
The benefits of recreational exercise are not distinct from that prescribed as part of a therapeutic intervention. Exercises can be prescribed to facilitate weight loss, preserve joint range of motion, improve strength, improve functional performance, and reduce symptoms. People are usually encouraged to partake in a low-impact aerobic exercise program e.g. walking, cycling, swimming or other aquatic exercise. Aquatic exercise may be preferable to land-based exercise for knee osteoarthritis as the body’s buoyancy greatly limits the compressive load that the knee must sustain. Seated cycling can also partially unload the knee and keep it stable while it is exercised through a large range of motion. The reason for promoting low-impact exercise is that it will encourage the benefits of exercise whilst avoiding the potentially damaging influences of high-impact activities.
At Bend + Mend in Sydney’s CBD we can prescribe a range of different exercise regimes to help you manage your arthritis and reduce pain. So don’t hesitate to come in and see how we can help manage your joint arthritis.