Have you ever experienced pain in the front of your knee?
Anterior knee pain can be caused by a number of anatomical structures, one such structure is the Patellar Tendon.
If you are unsure what tendon pain is, there is a fantastic Blog by B+M Physio Blake detailing 5 important facts for tendon pain that you should read up on!
In this blog we will be focusing on Patellar Tendon pain; What it is? What causes it? And how to best manage it.
Patellar Tendinopathy is a debilitating musculoskeletal condition which can often result in significant periods of absence from sport and potential early retirement from sport. Research into the condition has shown that one third of athletes who present with patella tendinopathy were unable to return to sport within 6 months (1) and 53% of athletes with this condition were forced to retire from sport (2).
The condition affects primarily young athletes (15-30), especially men, who participate in sports such as basketball, volleyball, tennis, athletic jumping events and football (3).
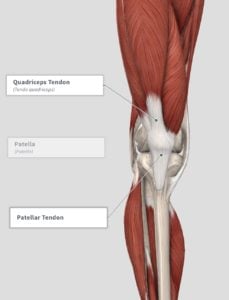
To understand patellar tendinopathy we will need to discuss the anatomy of the knee. The quadriceps muscles are connected to the inferior pole of the patella (kneecap) by the common quadriceps tendon through the patella. The patella tendon then connects the bottom of the patella to the tibial tuberosity (top of shin). The force generated by the quadriceps muscles act through the patella, causing the knee to extend.
What is Patella Tendinopathy?
Patella Tendinopathy is a source of anterior knee pain, characterised by localised pain at the inferior pole of the patella (Kneecap). Pain is often aggravated by loading (running, jumping) and increased with the demand of the knee extensor musculature (quadriceps), notably in activities that store and release energy in the patella tendon. The power needed for jumping, landing, cutting and pivoting requires the patella tendon to repeatedly store and release energy (4), similar to a spring. Repetition of this spring like activity over a single exercise session, or with insufficient rest to enable remodelling between training sessions can induce pathology and change in the tendons mechanical properties (7).
Tendinopathy specific symptoms include:
- Pain localised to the inferior pole of the patella (5).
- Tendon pain often occurs instantly with loading and usually ceases almost immediately when load is removed (6).
- Pain is rarely experienced in a resting state (6).
- Pain may improve with repeated loading (the “warm-up” phenomenon), but there is often increased pain the day after these energy storage activities.
- Aggravating activities include walking down stairs or decline squatting.
- Other symptoms such as pain with prolonged sitting, pivoting, squatting, and stairs may be present but are also features of patellofemoral knee pain and potentially other pathologies.
How can we treat Patella Tendinopathy?
At Bend + Mend we will provide you with an accurate diagnosis of the stage of tendinopathy, through a detailed questioning of the history of symptoms and your exercise history. Additionally, a thorough examination of the entire lower extremity is necessary to identify relevant deficiencies at the hip, knee and ankle. Often observed traits include, muscle wasting of gluteus maximus, quadriceps and calf.
There is currently good research to best manage patella tendinopathy, which should focus on progressively developing load tolerance of the tendon, as well as addressing key biomechanical risk factors (7).
While it may be helpful in short term for passive modalities (manual therapy, ultrasound, shockwave therapy, PRP injections) to assist with pain management, there is no evidence to show they are able to normalise tendon matrix or muscle tissue to address other deficits throughout the lower extremity (8).
Therefore a 4-stage loading program has been proposed to manage patellar tendinopathy. This involves a progressive loading program for the tendon, the stages of rehabilitation are (7):
- Isometric Exercises
- Isotonic Exercises
- Energy Storage Exercises
- Return to Sport Exercises
In following Blogs, I will progress through the stages of loading programs and give exercise options for each exercise stage.
If you are experiencing any anterior knee pain, you will benefit greatly from a Bend + Mend physiotherapy assessment and management plan to help you return to pain free daily living and exercise.
References:
- Cook JL, Khan KM, Harcourt PR, Grant M, Young DA, Bonar SF. A cross sectional study of 100 athletes with jumper’s knee managed conservatively and surgically. The Victorian Institute of Sport Tendon Study Group. Br J Sports Med. 1997;31:332-336.
- Kettunen JA, Kvist M, Alanen E, Kujala UM. Long-term prognosis for jumper’s knee in male athletes. A prospective follow-up study. Am J Sports Med. 2002;30:689-692.
- Lian ØB, Engebretsen L, Bahr R. Prevalence of jumper’s knee among elite athletes from diferent sports: a cross-sectional study. Am J Sports Med. 2005;33:561-567
- Alexander RM. Energy-saving mechanisms in walking and running. J Exp Biol. 1991;160:55-69.
- Blazina ME, Kerlan RK, Jobe FW, Carter VS, Carlson GJ. Jumper’s knee. Orthop Clin North Am. 1973;4:665-678
- Rio E, Moseley L, Purdam C, et al. The pain of tendinopathy: physiological or pathophysiological? Sports Med. 2014;44:9-23.
- Malliaras, Peter & Cook, Jill & Purdam, Craig & Rio, Ebonie. (2015). Patellar Tendinopathy: Clinical Diagnosis, Load Management, and Advice for Challenging Case Presentations. The Journal of orthopaedic and sports physical therapy. 45. 1-33.
- Gaida JE, Cook J. Treatment options for patellar tendinopathy: critical review. Curr Sports Med Rep. 2011;10:255-270